Outstanding cancer care requires an unparalleled team. Our specialists in medical oncology, chemotherapy, radiation medicine, pathology, surgical oncology, reconstructive surgery and radiology all work and consult together to deliver you the most effective treatments.
Markey has the region’s only team of breast fellowship-trained surgeons, who specialize in caring for the unique needs of breast cancer patients.
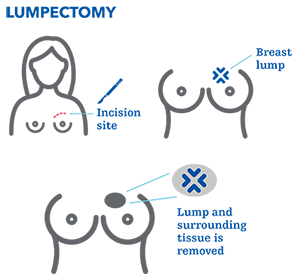 Lumpectomy (breast-conserving surgery). During a lumpectomy, your surgeon takes out only the cancer lump and an edge (margin) of healthy tissue around it, while the breast itself remains intact. If you are a woman with small breast cancer that has not spread, breast-conserving surgery may be a preferred option for you. Many women prefer this surgery instead of having their whole breast removed.
Lumpectomy (breast-conserving surgery). During a lumpectomy, your surgeon takes out only the cancer lump and an edge (margin) of healthy tissue around it, while the breast itself remains intact. If you are a woman with small breast cancer that has not spread, breast-conserving surgery may be a preferred option for you. Many women prefer this surgery instead of having their whole breast removed.
- Following the procedure, radiation therapy is recommended to kill cancer cells that may not have been removed during the surgery.
- Hidden Scar breast surgery. In some cases, women undergoing a lumpectomy will opt for Hidden Scar breast cancer surgery, which uses a single incision in a hidden area to remove the cancerous tissue. With this option, visible scarring is reduced and the breast retains its natural shape.
- Mastectomy (removal of the entire breast). The doctor may advise a mastectomy for women with any of the following:
- Cancer that is too large for breast conservation or is in multiple locations in the breast.
- Previous radiation therapy to the affected breast or chest area.
- Two or more areas of cancer in the same breast that are too far apart to be removed with one incision.
- Breast that is very small and tumor that is large.
- Inflammatory breast cancer.
- Connective tissue disease(s) for which there is a contraindication to radiation therapy.
- A current pregnancy, because radiation normally needed after breast-conserving surgery could harm the unborn baby.
- Surgical margins that are not “clear” – or free of cancer – after a lumpectomy.
There are three types of mastectomies:
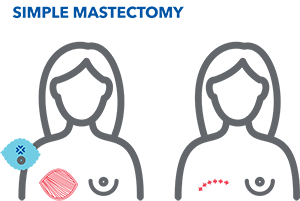
- Total (or simple) mastectomy. This type removes the whole breast and often the lining over the chest muscle.
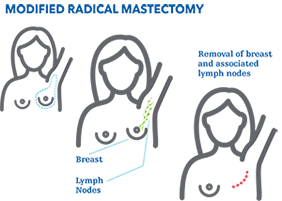
- Modified radical mastectomy. This type removes the whole breast, most of the lymph nodes under the arm and often the lining over the chest muscles.
- Radical mastectomy. This is also called a Halsted radical mastectomy. This type of mastectomy is reserved for rare cases. The surgeon removes the breast, the lymph nodes under the arm, the lining over the chest muscles and both of the chest muscles under the breast.
Breast reconstruction is surgery to create a new breast in place of a breast that has been removed during mastectomy. A breast mound is created that comes as close as possible to the shape and look of a natural breast. The surgery may be performed to reconstruct either one breast or both breasts.
What Are Lymph Nodes?
Breast cancer can spread to the rest of the body by first spreading to the patient’s lymph nodes. Lymph nodes are small, bean-shaped structures within a body’s immune system collecting fluid, waste material and more outside the bloodstream.
Cancer in the lymph nodes can be hard to notice, but in the case of an infection, inflammation or cancer, these nodes can grow larger and present themselves as an area of interest during cancer screening. A sentinel lymph node is defined as the first node to which cancer cells are most likely to spread from a primary tumor. The surgeon finds the sentinel lymph node by performing the sentinel lymph node procedure. This is performed in the operating room by injecting the breast with a radioactive substance and/or blue dye. The surgery is done at the same time as the surgery on the breast.
The number of cancer cells in the lymph node and the number of involved lymph nodes are of key interest. In the case of very few cells in a lymph node, it may not change the treatment plan at all. But the more cancer there is in a node, the more likely it is that the cancer is growing and likely to spread, in which case your doctors will adjust the treatment plan accordingly. In some cases where the cancer has spread to the lymph nodes, your doctor may recommend removing most of the lymph nodes under the arm.
Making a Decision About Reconstruction
The decision to have breast reconstruction is a personal one. It depends on how you think you will feel after a mastectomy. If you think you would feel uncomfortable with a flat chest or wearing a false breast (prosthesis), you may consider breast reconstruction. If you do not want to have any more surgeries, you may choose to forgo it.
If you are considering breast reconstruction, talk with your doctor about it before your mastectomy. Your doctor can tell you whether reconstruction is an option for you and, if so, what type of reconstructive surgery is suggested for your circumstances. Breast reconstruction is covered by most insurance providers, including Medicare and Medicaid in Kentucky, according to The Women’s Health and Cancer Rights Act of 1998. Reconstruction can be performed at the time of your mastectomy or at a later date.
Factors affecting the type that is recommended for you can include:
- The size and location of the cancer, which determines the amount of skin and tissue to be removed in the mastectomy
- The amount of tissue removed from the breast
- If your chest tissue has been damaged by radiation therapy or aging and is not healthy enough for reconstruction surgery
- Potential for complications
- Your overall health and medical history
Once again, be sure to discuss the common risks with your doctor before deciding.
What Are the Different Types of Breast Reconstruction?
There are two main types of reconstruction surgery:
- Expander/implant. An expander is used to create a breast mound and expand the skin and muscle to allow the placement of a filled breast implant.
- Autologous tissue. A person’s own body tissues are used to reconstruct a new breast mound. Reconstruction surgeries leave you with two surgical wounds: the chest and the site where tissue was removed.
You may also decide to have other procedures to improve how your new breast shape looks.
Oncoplastic Surgery
Oncoplastic surgery is a single procedure that combines cancer surgery and plastic surgery for breast cancer patients. This procedure aims to remove the area of the breast containing cancer followed by reshaping the remaining breast tissue to normal appearance.
Not all patients undergoing a form of breast conservation surgery will require this procedure. Ask your breast surgeon to learn about your personal needs in breast cancer care.
Healing After Surgery
Immediate reconstruction surgery has a longer recovery time than for mastectomy alone. With autologous tissue surgery, a second surgery site will need to be cared for as it heals.
It can take several months before results of breast reconstruction can be seen. Be patient as your body heals.
Chemotherapy is one of the longest used and most common treatments for cancer. In most cases, chemotherapy works by interfering with the cancer cell's ability to grow and reproduce. For some cancers, chemotherapy may be used alone or combined with other treatments such as radiation or surgery. A combination of chemotherapy medicines is typically used to fight a specific cancer.
While chemotherapy can be quite effective in treating certain cancers, the medicines reach all parts of the body, not just the cancer cells. Many side effects can occur, and being prepared can help you and your caregivers manage them effectively.
How Is Chemotherapy Given?
Chemotherapy can be given in various ways, such as:
- A pill to swallow
- An injection (shot) into the muscle or fat tissue
- Directly into the bloodstream, or intravenously (also called IV)
- Topically (applied to the skin)
Chemotherapy is usually given in cycles to allow healthy cells the time to recover. Treatment may be given daily, weekly, every few weeks or monthly, depending on your situation.
Chemotherapy is usually given in an outpatient setting. This includes a hospital, clinic or healthcare provider's office.
Patients are encouraged to bring something comforting to their treatment. Since it is hard to predict how a patient will feel afterward, the patient should arrange to have someone drive them to and from their appointment.
Radiation therapy is a treatment for cancer that uses high-energy X-rays. A machine directs the rays to the area of cancer, with a goal to kill or shrink cancer cells.
Radiation is most often used along with other breast cancer treatments, like surgery or chemotherapy. Your doctor may advise radiation if:
- You have an early-stage breast cancer. This is called adjuvant treatment. Radiation is often used after breast-conserving surgery. It is sometimes used after mastectomy. The goal is to kill cancer cells that cannot be seen, but may have been left behind after surgery, which lowers the chance the cancer will come back.
- You have metastatic breast cancer. This means the cancer has spread. The goal of radiation in this case is mainly to ease symptoms of the cancer. This is sometimes called palliative treatment.
Types of Radiation Therapy
- External radiation. This is also known as external beam therapy (EBRT). It is the most common type used to treat breast cancer. This treatment sends high levels of radiation directly to the cancer cells. Since radiation is used to kill cancer cells and to shrink tumors, special shields may be used to protect the tissue surrounding the area being treated.
- Internal radiation. This is also known as brachytherapy or implant radiation. This type of radiation treatment is given inside the body in the area of the cancer. It gives a higher dose of radiation to a small area for a shorter time. The radiation source may be put directly into the area of the breast tumor, or it may be put in through a small tube placed near the tumor.
Visit our Radiation Oncology website for an overview of services.



























