CAR T-Cell Therapy

At the UK Markey Cancer Center, we have Kentucky’s largest CAR T-cell therapy program — and we were the first in the Commonwealth to adopt this groundbreaking treatment in 2018.
We’re a national leader in CAR T-cell therapy (also called chimeric antigen receptor T-cell therapy), which harnesses your body’s immune system to fight blood cancer. This advanced treatment offers long-term remission or even a cure for some patients.
Experience matters
Experience with your specific cancer matters when it comes to advanced treatments like CAR T-cell therapy. It’s a complex process and you need a knowledgeable team that knows all the ins and outs of the procedure. Markey has the advanced capabilities and experienced team to deliver you this transformative treatment.
Not that long ago, CAR T-cell therapy was an experimental therapy only offered through clinical trials at Markey and other select hospitals. Thanks to our pioneering research, CAR T-cell therapy is now a standard treatment for many blood cancers. And it has the potential to treat an even wider variety of cancers.
At Markey, we’re at the forefront of CAR T-cell therapy, conducting most of the CAR T procedures in Kentucky. In fact, we’ve performed over 100 CAR T-cell transplants — a large number for such a specialized and relatively new treatment. And while CAR T-cell therapy is new, we’ve been here caring for people with blood cancers for over 40 years.
Why choose Markey for CAR T-cell treatment?
Markey is Kentucky’s NCI Comprehensive Cancer Center. The NCI designation is the highest honor reserved for institutions redefining the future of cancer prevention and treatment. At Markey, you will find in one place:
- Access to groundbreaking research and clinical trials for your specific blood cancer
- World-renowned experts in your type of blood cancer
- The latest treatments, like CAR T-cell therapy
Here’s what else sets our CAR T-cell program apart:
- National recognition: U.S. News & World Report has recognized Markey as a top hospital every year since 2017. We're also listed among the publication’s highest-ranked performers for leukemia, lymphoma and myeloma treatment.
- The highest cell therapy accreditation: Our program is accredited by the Foundation for the Accreditation of Cellular Therapy. This endorsement signifies we meet rigorous quality and patient safety standards.
- Unmatched expertise: Our team includes specialists in your blood cancer, oncology nurses, cancer pharmacists, CAR T-cell therapy coordinators and more. We only treat blood cancers. This specialized focus ensures you receive expert care and more treatment options.
- Compassionate care: Cancer treatment brings challenges that can be difficult to cope with. Your care at Markey goes beyond the details of your treatment plan. We are here to support your physical, emotional and mental well-being.
- Partners with referring physicians: As a referring physician, you can trust Markey to care for your patients when they need CAR T-cell therapy. We’ll keep you informed and ensure a smooth transition back to your care once your patients complete their treatment.
Clinical trials that give you more treatment options
At Markey we're not settling for today’s treatments. We’re developing the treatments of tomorrow and pushing the boundaries of CAR T-cell therapy by offering access to innovative clinical trials.
Our research includes exploring new treatments to fight a wider range of cancers. We’re also investigating "off-the-shelf" CAR T products that could provide faster, more readily available treatments for blood cancers. And we’re looking at ways to combine CAR T treatment with other therapies to improve treatment results.
Your doctor may let you know if a clinical trial is an option for you. And be sure to ask us if you’re interested in participating in a trial. Search our clinical trials.
Types of cancer we treat with CAR T-cell therapy
In only a short time, CAR T-cell therapy has revolutionized treatment for many blood cancers. It could one day do the same for solid tumors, including kidney cancer, lung cancer and bone cancer.
The blood cancers we treat with CAR T-cell therapy include:
How does CAR-T cell therapy work?
Your immune system is naturally equipped to fight cancer. But cancer cells are tricky. They can outmaneuver and overwhelm your body’s defense system, allowing cancer to grow and spread.
CAR T-cell therapy is an innovative type of immunotherapy that uses T-cells, a type of white blood cell your body uses to fight infections.
During CAR T-cell therapy, we extract T-cells and send them to a lab, where they’re reengineered to provide them with instructions to find and kill cancer cells. These modified T-cells, called CAR T-cells, can last in the body for years and provide long-term benefits.
What to expect
Make an appointment with us if you’re diagnosed with blood cancer or considering CAR T-cell therapy. The earlier we see you, the more treatment options you may have.
At your first appointment, you’ll meet with your blood cancer specialist. Your doctor will perform an evaluation and discuss possible treatments with you. If CAR T-cell therapy is a good option, you’ll need tests to tell us if you’re healthy enough for the treatment.
Throughout your treatment, you’ll have a specialized team of blood cancer experts, oncology nurses, cancer pharmacists, CAR T-cell therapy coordinators and more. Your team focuses exclusively on blood cancers and will be with you every step of the way.
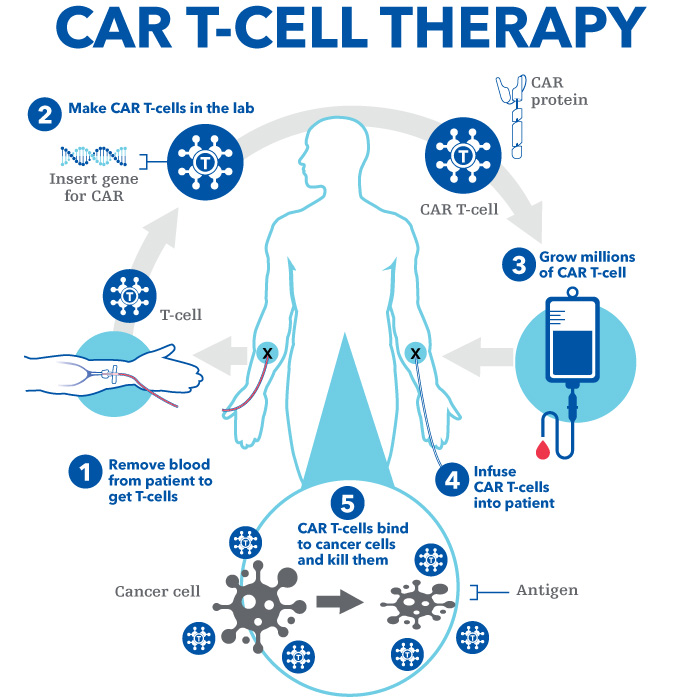 Here’s what to expect during CAR T-cell therapy:
Here’s what to expect during CAR T-cell therapy:
T-cell collection: We collect your T cells by drawing blood from a vein in your arm. The blood goes into a special machine that collects the T cells. This process is called apheresis. After removing the T cells, we return the blood to your body. This simple process takes several hours.
Manufacturing: Your T-cells go to a lab that modifies them to fight cancer and then creates millions of new CAR T-cells. These newly engineered cells know how to seek out cancer cells and destroy them.
Chemotherapy: While the lab prepares your CAR T-cells, you may receive chemotherapy to keep your cancer in check. Not everyone needs this “bridging” chemotherapy.
Infusion: Before you get your new CAR T-cells, you’ll get a low dose of chemotherapy. This treatment gets your body ready for the CAR T-cells. We then return the CAR T-cells to your body via an IV infusion.
Hospital stay: You'll need to stay in the hospital for about 10 days after your procedure so our team can watch you for side effects. You’ll stay on a special floor of the hospital dedicated to patients getting treatment for blood cancer.
Return to home: You’ll need 24/7 caregiver support for at least 30 days after your procedure. It’s important to make sure you have support from a loved one before you start treatment. You’ll get instructions, and we’ll explain the side effects to watch for before you leave the hospital.
Follow-up care: You’ll have regular follow-up appointments at Markey so we can see how the cancer responds to treatment. After a follow-up period, you can resume care with your regular hematologist or oncologist while still having some appointments at Markey.
What are the possible side effects of CAR T-cell therapy?
CAR T-cell therapy is a powerful cancer treatment, but it can cause side effects. We are vigilant in finding these side effects and treating them if they do happen. Most symptoms do go away.
Let us know right away if you experience these side effects:
- Cytokine release syndrome: CRS is widespread inflammation caused by your immune system attacking cancer cells. Symptoms may include fever, fatigue, rapid heartbeat and difficulty breathing.
- Neurotoxicity: Nervous system symptoms may include confusion, dizziness, difficulty speaking and trouble concentrating or staying awake.
Patient resources
Markey offers comprehensive support services to help you during your treatment. Let us know if you need help. Our team provides mental health counseling, nutrition guidance, transportation and temporary lodging assistance and more.
We also offer transplant support groups. Patients in these groups have gone through CAR T-cell therapy or other types of transplants and can share their experiences with you. It can help if you have someone to talk with who’s been through the process and understands.









