Lexington woman aspires to empower fellow pulmonary hypertension patients

When Nicole Creech was diagnosed with pulmonary hypertension 11 years ago, she first thought she could manage it all on her own.
“I didn’t want to know anybody else with it,” she said. “I didn’t want to meet anybody that had been diagnosed with it. I really just wanted to be left alone and go on with my life.”
But Creech later realized how uplifting it is to receive encouragement from people who understand the disease and have walked in her shoes before. She is now on a mission to spread the word and help others like her who are living with this rare chronic lung disorder.
Having a condition like pulmonary hypertension can be isolating, Creech said, because so few have it or are even familiar with it. Pulmonary hypertension is a type of high blood pressure that affects the lungs: The arteries carrying blood from the heart to the lungs become so narrowed and damaged that the right side of the heart is forced to work harder just to pump blood. If left untreated, pulmonary hypertension can often be fatal within a few years.
Treatments that manage symptoms are helping people like Creech live longer, and she wants to give hope to others and let them know they’re never alone.
A pulmonary hypertension diagnosis
Like many with pulmonary hypertension, Creech suffered for several years before she got the right diagnosis. Creech had shortness of breath and fatigue that made it hard to simply wake up in the morning. Many people are often incorrectly diagnosed with asthma, allergies or a heart murmur, among other conditions. Creech’s symptoms came and went for about three years before she couldn’t ignore them any longer.
On the Fourth of July weekend in 2008, Creech began to sweat profusely and couldn’t even walk a short distance without feeling like she might pass out. She rushed to the UK Chandler Hospital Emergency Department, where doctors saw that something was very wrong.
“I couldn’t breathe. I felt like I was suffocating,” she remembered. “I must’ve looked horrible because they put me on oxygen immediately.”
Creech was in the hospital for 21 days, and the prognosis wasn’t encouraging: There is no cure for pulmonary hypertension. Treatments focus on relieving symptoms and prolonging survival, and she was told she would live five years with treatment.
“The initial shock of it was one thing,” she said. “Inside, I was scared, but there was something that said, ‘This isn’t gonna happen. You’re gonna beat this. You’re gonna be fine.’”
Ongoing treatment for pulmonary hypertension
During Creech’s three-week hospital stay, Dr. David Booth of the UK Gill Heart & Vascular Institute placed a catheter into a vein in her chest. The catheter allows Creech to insert medication daily using a syringe into a small battery-powered pump, which continuously supplies the medicine.
“There are no words to really describe that man,” she said tearfully of Booth. “He literally saved my life. I feel blessed that he is my doctor.”
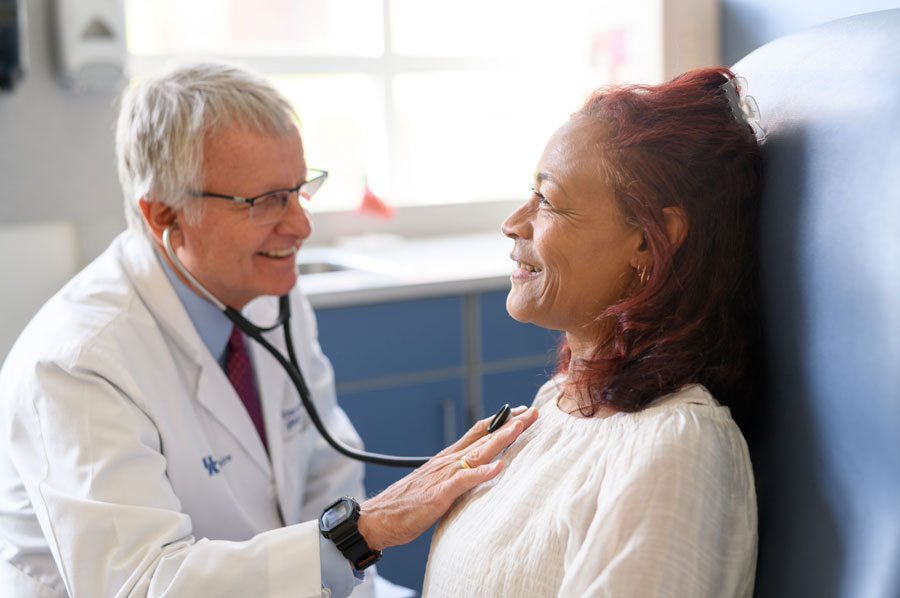
According to Booth, a heart catheterization when Creech was first diagnosed in 2008 showed severe pulmonary hypertension. But a catheterization performed just a year ago showed her pulmonary arterial pressure as essentially normal.
“The reason she’s done so well is that we were able to lower her pressures to normal range with drug therapies. The right side of the heart doesn’t have such a hard job,” Booth said.
In other words, the medication works well for Creech. It’s rare for it to work that well, though, Booth explained. Creech takes Flolan, or epoprostenol GM, which was the standard treatment for critically ill patients like Creech when she was first diagnosed. Although it’s still the standard today, some patients with less severe symptoms use oral medications, Booth said. UK HealthCare is the only healthcare system in the region offering expertise in the management of pulmonary hypertension.
A busy life helping others
Eleven years later, the 47-year-old Creech, who lives in Lexington with her Yorkshire terrier, is still fighting. She sleeps with oxygen at night and still experiences fatigue and shortness of breath, as well as a few other symptoms.
Even though she needed to retire from her job in property management, that doesn’t mean she isn’t busy. She leads the UK Pulmonary Hypertension Support Group. Ten patients attended the first UK support group meeting a few years ago, and it proved to be an eye-opening experience for everyone, Creech included.
“It was the first time many of us had ever seen one person, let alone nine other people, with pulmonary hypertension in one place,” she said.

Kim Jackson, RN, a nurse coordinator at the Pulmonary Hypertension Clinic at the Gill Heart & Vascular Institute, said pulmonary hypertension patients really benefit from the extra support they receive in a group setting.
“Pulmonary hypertension is a frightening disease because by the time we get the patient, they're usually pretty sick because it’s misdiagnosed so much,” Jackson said. “It’s good for them to talk to somebody that’s going through the same thing they’re going through.”
Giving pulmonary hypertension patients hope
Creech organizes sponsors and speakers, topics, and discussions for the UK support group.

“We want to empower people with hope,” she said. “It’s really important to know that there is support available. It’s such a rare disease. You think that means there’s nobody close like you, but that’s not the case.”
The UK group is a local branch of the national Pulmonary Hypertension Association. Creech sits on the national association’s support group leader advisory board and was recently asked to join its board of trustees.
As the UK support group leader, she visits newly diagnosed people in the hospital, which gives her a sense of purpose and drive to continue her mission.
“I need to keep moving and fighting for a cure,” Creech said. And she likes the realization she sees in a patient’s eyes when she walks into the hospital room, smiling and happy. “They have hope that they might be OK.”
Creech also does home visits, especially for older patients who can’t make it to meetings, and she meets with parents whose children have the condition.
“This is another one of those chronic illnesses that doesn’t discriminate,” she noted. “Our group is growing. We have people newly diagnosed all the time.”
Additionally, she uses Skype, Facetime and a Facebook group to connect with patients and is hoping to do a Facebook live meeting at some point.
Jackson feels that Creech is a great ambassador for the support program. “She just has this way about her that makes people feel comfortable,” she said. “We’re lucky to have her, and I think the group is lucky to have her.”
At the time of Creech’s diagnosis, there were only a handful of medications used to treat pulmonary hypertension. Now, many more options and clinical trials at UK and beyond are available.
Even though she already does so much to support her fellow patients, Creech still wants to do more, including fundraising and advocacy for additional research funding. “There’s definitely more for me to do,” she said. “I’m just getting started.”
To find out more about the UK Pulmonary Hypertension Support Group, contact Nicole Creech at nmcreech@gmail.com or 859-321-3816.





