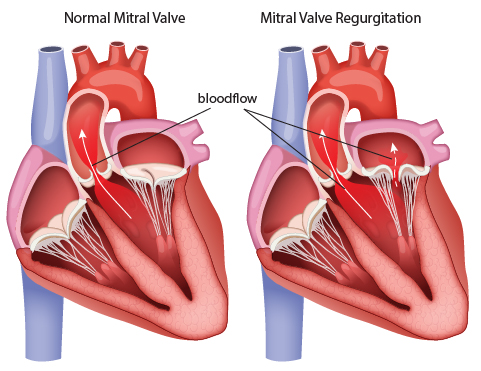
 The left side of the heart pumps oxygenated blood from the lungs to the rest of the body. Blood flows from the upper chamber or left atrium down through the mitral valve to the left ventricle with each heartbeat.
The left side of the heart pumps oxygenated blood from the lungs to the rest of the body. Blood flows from the upper chamber or left atrium down through the mitral valve to the left ventricle with each heartbeat.
Mitral valve regurgitation occurs when the valve on the left side of the heart does not close completely, allowing blood to leak back through to the left atrium. Mitral valve regurgitation can cause the heart to work harder.
There are two types of mitral valve regurgitation:
- Primary mitral valve regurgitation is caused by disease in the leaflets that open and close with each heartbeat.
- Secondary mitral valve regurgitation is due to disease in the left ventricle or left atrium.
It is common for people to have mitral valve regurgitation with no symptoms. Some people live with mild symptoms their whole lives, while others notice symptoms that come on suddenly after a cardiac event, such as a heart attack or infection of the valve.
Signs of mitral valve regurgitation include:
- Coughing
- Exhaustion or fatigue
- Feeling your heart beating or having a rapid heartbeat
- Shortness of breath when lying down or during activity
- Difficulty sleeping flat or feeling like you need to prop yourself up on pillows due to smothering or shortness of breath
- Waking up an hour or so after going to sleep due to difficulty breathing
Conditions that can damage heart valves increase the risk of mitral valve regurgitation. Primary risk factors include:
- Coronary heart disease
- Heart valve infection
- High blood pressure
- Mitral valve prolapse, or malfunction of the mitral valve
- Swelling in the lower chamber of the heart
Rheumatic heart disease, a complication of untreated strep throat, is a risk that is becoming less common. Other rare risk factors are Marfan syndrome, an inherited condition that can affect heart valves, and untreated syphilis.
Having used the recalled diet pill Fen-Phen (fenfluramine and phentermine) or dexfenfluramine is also a risk factor for mitral valve regurgitation.
Your first visit to the structural heart program at the UK Gill Heart & Vascular Institute will be a meeting that often takes only an hour. During this appointment, you will meet your care team, including:
- Your interventional cardiologist, a specialist who uses catheter-based procedures to diagnose and treat heart issues
- An advanced practice provider, (a physician assistant or nurse practitioner)
- A nurse coordinator
- A patient navigator, who works with you to help ensure that your healthcare needs are met
If you need imaging, you will be scheduled for a follow-up visit at this time.
For the visit:
- Wear comfortable clothing.
- Bring your insurance information. While UK HealthCare accepts all insurers, not every insurer is in network.
- Bring a list of all medicines and supplements you currently take.
- You may find it helpful to have a family member or friend with you at this visit.
Where we are located
The UK Gill Heart & Vascular Institute is located at 800 Rose St. in Pavilion G, on the first floor of UK Albert B. Chandler Hospital. We will mail you a map and directions when your appointment is scheduled.
Patient drop-off
Patients can be dropped off in front of the main entrance to Albert B. Chandler Hospital at 1000 S. Limestone. If you are dropped off at the main entrance, you’ll enter the revolving doors on the ground floor of the hospital. Take the main stairs just to the left (or elevator across the atrium) to the first floor of Pavilion A.
After climbing the stairs or taking the elevator, turn left. You’ll pass the Kentucky Wall and Kentucky Children’s Hospital on your right. Continue to the end of the hall until it comes to a T shape. Turn left and the Gill clinic entrance is across from an open area housing the organ donor wall.
Parking
It is easiest to park in the UK HealthCare Parking Garage, across from the hospital at 110 Transcript Ave.
There are two paths from this garage to the Gill clinic:
- You may take the free shuttle from Level A of the parking garage. You’ll exit the shuttle at the Pavilion A/ Pavilion G stop in front of the main entrance to the hospital. After climbing the stairs or taking the elevator, turn left. You’ll pass the Kentucky Wall and Kentucky Children’s Hospital on your right. Continue to the end of the hall until it comes to a T shape. Turn left and the Gill clinic entrance is across from an open area housing the organ donor wall.
- From Level C of the parking garage you may walk or take a golf cart across the pedway to the first floor of Pavilion A. Turn left past the help desk and walk away from the dining hall. You’ll pass the Kentucky Wall and Kentucky Children’s Hospital on your right. Continue to the end of the hall until it comes to a T shape. Turn left and the Gill clinic entrance is across from an open area housing the organ donor wall.
If you need help finding your way, information desks are located inside the main entrances to Pavilion A, both on the ground floor and at the end of the pedway on the first floor. You may also call the information desk at 859-323-5816.
The UK Gill Heart & Vascular Institute’s structural heart program offers patients access to advanced clinical trials. Our Cardiology Clinical Research Center gives structural heart disease patients a chance to try new technologies years before they are available to the general public. These innovative and potentially lifesaving procedures are not available at other facilities in the region.











