Family found answers at Kentucky Children’s Hospital when infant daughter developed mysterious illness

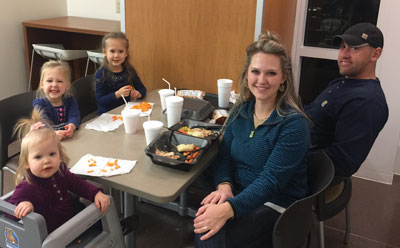
A hospital cafeteria would seem to be the last place where a family would willingly choose to spend time on Thanksgiving. But for the Watts family of Harrodsburg, Kentucky, the cafeteria that serves families, visitors and employees of Kentucky Children’s Hospital was the ideal place for them to celebrate the true spirit of the holiday.
For just a year before – in November 2016 – their 6-month-old daughter Jade had fallen severely ill and had been hospitalized upstairs, in the Pediatric Intensive Care Unit (PICU), with infant botulism, a rare condition that afflicts approximately 100 children each year. The expert knowledge, and tender care, shown by emergency and PICU staff at Kentucky Children’s Hospital restored Jade to health and represented, for the Watts family, the perfect reason to return and give thanks.
Warning signs
As the mother of three older girls, Courtney Watts knew something was not right with Jade as the hours passed on Nov. 17, 2016. Up to that point, Jade had been a healthy baby who had hit all of her developmental milestones. But on this day, Jade had no appetite and struggled to nurse.
“There was no fever, no rash. She wasn’t acting different in any other way,” Courtney said. “But by bedtime, she was gagging and coughing during nursing. I was worried she would become dehydrated. I decided that if she didn’t wake up ravenous the next morning, we would go straight to the pediatrician’s office.”
The next morning it was clear Jade was worse. “She was alert and happy to see me, but she was oddly weak,” Courtney recalled. “She could neither latch on nor swallow during nursing, but she was too weak to push me away.”
Courtney and her husband, Casey, were at the pediatrician’s doorstep with Jade when the nurse unlocked the door at 8 a.m. and informed them there would be at least an hour wait. Upon hearing Jade’s raspy, faint cry and seeing her full-body weakness, the nurse instructed them to go to the UK Makenna David Pediatric Emergency Center at Kentucky Children’s Hospital immediately. “I felt like there was a hand wrapped firmly around my throat,” Courtney said. “There was something wrong with my baby.”
Connecting mom to mom
As emergency nurse Renee Spradlin, BSN, started Jade’s IV, she noticed something alarming. “Usually, if we need to place IVs for children, you get a cry or scream,” Spradlin said. “But Jade didn’t react. No crying, no tears. She just laid there. It’s scary when a baby does not react at all.”
That IV needle prick was just the first in a succession as the emergency staff tried to pinpoint the cause of Jade’s increasing weakness and continuing decline. They inserted a catheter to test for the usual suspect of a urinary tract infection: negative. They drew blood to screen for an elevated white blood cell count: negative. They performed a lumbar puncture to test for meningitis: negative. They conducted a cranial CT scan to check for bleeding in her brain: normal.
“My baby had just been pricked and poked and prodded from every angle,” Courtney said. “Nothing showed up. Nobody could tell us what was wrong. It was an absolutely gut-wrenching feeling.”
Now that I have a child of my own, I have even more empathy for the parents who come in with their sick children. I know that it makes a big difference in their care.”—Renee Spradlin, BSN
As one test followed another, Courtney was grateful for Spradlin’s support. “She connected with me on a mom level,” she said. “I needed a mom to understand this was MY baby on the table. This was MY heart and soul being pierced with every needle she took, every gouge her body endured. I trusted the doctors and their expertise, but I needed another mom to love my baby like she was hers, and that is what Renee did.”
It came naturally to Spradlin; all she had to do was imagine her son, Matthew, in the same position. “I’ve worked as an emergency room nurse for seven years,” she said. “Now that I have a child of my own, I have even more empathy for the parents who come in with their sick children. I know that it makes a big difference in their care.”
“In the place where we needed to be”
As Jade was wheeled up to the 12-bed PICU, Courtney looked at her daughter’s tiny, limp body on the gurney equipped with a crash cart, the emergency equipment needed in case a patient’s heart stops. “It was so surreal to be in this situation,” she recalled. “We were supposed to be having a regular day. I kept thinking, ‘How did this happen? What did I miss?’”
For Jade’s first 45 minutes in the PICU, her parents waited in the Ronald McDonald family room while her care team settled Jade into her room. “It was hard to be away from her,” Courtney said. “But I felt like we were in the place we needed to be. I felt that if there were people in the world who could solve this problem, they were the people in the room right then looking at my baby.”
The couple kept busy answering a flurry of questions and helping construct a timeline of Jade’s previous few days. The doctors were especially interested in one question: When was Jade’s last bowel movement? As Courtney thought back over the week – Jade was with her babysitter one day, with her grandmother another day – she realized it was possible that the last time was Monday, four days before.
“I could tell they were on the trail of something,” Courtney said. “They were figuring things out.”
Mystery solved
They were. The PICU team had called in Robert Broughton, MD, chief of pediatric infectious diseases, to consult on Jade’s case. After a quick review of Jade’s symptoms – weakness, flaccid muscle tone, constipation, poor nursing, weak cry – Broughton diagnosed her with infant botulism.
“There is no other condition quite like it,” Broughton said. “Jade had a characteristic presentation of it that made it easy to recognize.”
Infant botulism occurs when a baby – usually under six months of age – ingests Clostridium botulinum spores, which are found in soil and honey products. The spores germinate into bacteria that multiply in the intestine and release a toxin. This toxin circulates in the blood and binds to the neuromuscular junction, disrupting the transmission of electrical signals from the nerves to the muscles.
“That’s why patients develop weakness and can’t move well,” Broughton explained. “It also interferes with the smooth muscle in the gastrointestinal tract, which causes the hallmark constipation.”
Even though there are only around 100 cases of infant botulism each year – the majority of them in the United States – Broughton was no newcomer to the condition. He had encountered it firsthand multiple times throughout his 35 years of practicing medicine at UK.
“I was the chief resident in 1979 or 1980 when we had the first case here – the first case ever reported in Kentucky,” he recalled. “Since then, I have probably seen 20 cases. Even though it is a rare disease, you are more likely to encounter it at a tertiary medical center like Kentucky Children’s Hospital because we have patients referred to us from all over central and eastern Kentucky.”
Thanks to his expertise, Broughton knew the proper regimen to follow. To confirm his diagnosis, he took a stool sample that was shipped to the state diagnostic lab in Frankfort to be tested for the presence of the toxin. However, it can take 24 to 72 hours for those results.
Because of his high degree of certainty in his diagnosis, Broughton contacted the California Department of Health, which controls the distribution of the antitoxin used to treat infant botulism. He requested a dose of Baby BIG-IV (botulism immune globulin) be sent immediately. The nearest supply of the antitoxin was in North Carolina; it would be shipped overnight.
“The goal of the medicine is to prevent any further deterioration of the baby’s condition by absorbing the toxin in the bloodstream and neutralizing it before it can attach to the neuromotor junction,” Broughton said. “It shortens the course of the illness. However, it’s important to realize that the medicine cannot reverse the toxin that has already attached; that has to degrade over time. So, while the baby will not get any weaker after the medication, it may be a few days before parents see an improvement in their child’s condition.”
Holding their breath
When Courtney went home on Friday night, she felt hopeful. She now had a name for her daughter’s illness. The antitoxin was on its way and would be administered the next day. On Saturday morning, she returned to the hospital in an upbeat mood. It did not last long.
When she entered Jade’s room, she found her husband in a somber conversation with Matthew Bacon, MD, the pediatric critical care doctor on duty. Jade’s condition had deteriorated further overnight and she was starting to have difficulty breathing.
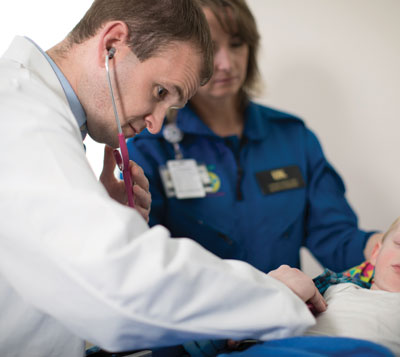
“When a child loses their muscle tone, they can’t protect their airways,” Bacon explained. “They can’t cough or clear their secretions. There’s a danger of them gagging or aspirating. Before her condition reached a crisis point, it seemed appropriate for us to intubate Jade proactively so that a ventilator could assist with her breathing.”
Jade’s parents were shaken by the news. “It hadn’t sunk in how fast and how much she was going to continue to decline,” Courtney said. They agreed to the intubation – with one request: that Jade’s father be allowed to remain in the room during the procedure.
“In pediatrics, we try to let the family in for all procedures,” Bacon said. “I gauge the family’s stress level and comfort level. I always tell them there is only one patient in the room at a time. So I was happy to let Casey stay and watch as much as he was comfortable. Jade did well, the procedure went smoothly, and it helped for Jade’s dad to see that.”
It was tremendously helpful for Jade’s mom, too. “I appreciated the ability of Dr. Bacon – and all the caregivers – to maintain their professionalism without losing their ability to connect with us as parents,” she said. “Dr. Bacon was in control, but he still gave us the room to be parents in a very powerless situation.”
Comforting company and care
After Jade received her antitoxin, the Watts family shifted from crisis mode to wait-and-watch mode for the next several days. As the long hours passed, they appreciated the care from the nursing staff. Trinaye Pierson, RN, who was training on the floor, entered Jade’s room with a song every time. “She brought life and sunshine into the room with her,” Courtney said. “She was so personal, so vibrant. She made you feel happy being around her.”
Pierson proudly admits that singing is big part of her approach to caregiving. “The hospital can be a scary place for kids,” Pierson said. “I know that my singing resonates with them. It calms them. Sometimes the parents enjoy it and join in, too.”
Courtney also formed a close bond with Ashley Kenley, RN, an 11-year-veteran of the PICU and Jade’s primary nurse for five days. Kenley looked at family photos and asked questions about Jade and her sisters to get to know the family better. She understood how painful it was for Courtney and Casey to see their small daughter attached to so many tubes and hoses and all alone there in the hospital bed. So when Courtney asked if she could hold Jade, Kenley made it happen.
“You think about, ‘What if something happened to your own child and you couldn’t hold her again?’” Kenley said. “I consulted with the attending physician, and we decided as a team it would be OK. I was so happy for them to have this very loving moment with their daughter and to feel that physical connection again.”
Kenley looked after not just Jade but her parents as well. She kept Courtney on a regular schedule for pumping her breast milk. She ordered them meals. She let Courtney – a dental hygienist – assist with Jade’s oral care as well as with baths, changing diapers, applying lotion, anything that enabled the mother to touch her daughter and assure her child of her presence.
“As a parent, I can understand the loss of control of caring for your child,” Kenley said. “It’s important to talk with parents about how they’re feeling about the situation, go through the plan of the day and answer any questions they have. We need to take care of the families, too.”
“We are all Team Jade”
At last, Jade turned a corner. The first signs of recovery were small: a flick of a hand, a slight movement of her foot. “The family was very understanding of the need to be patient with Jade’s body and to give her time,” said Asha Shenoi, MD, a pediatric critical care doctor in the PICU. “They were willing to work with us; we were all Team Jade.”
By Tuesday, November 22, Jade’s eyes were open and tracking her parents’ voices. She was moving her limbs. She was able to cough on her own – the key requirement in order to remove the ventilator. She was ready to be extubated. Kenley had traded shifts so she could be on duty for this major milestone in Jade’s recovery. She even gave the family a new outfit for Jade to wear on this special day.
“This was one of those times Ashley was so much more than a nurse to our family,” Courtney said. “To think that, after working a 12-hour-day, she sacrificed her free time and went to the mall to shop for our daughter, that was above and beyond. It shows that she’s caring for her patients whether she was on the clock or not.”
After Shenoi removed the breathing tube, Courtney was finally able to fully embrace her daughter again. “I felt like all was right in the world,” she said.
Not quite all was right with the world. During her first 24 hours off of the ventilator, Jade struggled to breathe deeply. “When we’re dealing with patients who are brittle, it is important for us to not just take intermittent snapshots but to get a continuous feel for the trend of the patient,” said Michael Wittkamp. “Since we are a smaller PICU, we are able to invest that time in our patients.”
That is exactly what respiratory therapist Richard Broaddus, RRT, did for Jade. For 30 years, he has worked strictly with pediatric patients; he knew exactly what Jade needed. “There is no magic pill for this,” he said. “It takes a lot of therapy and a lot of time in these situations.”
After monitoring her closely throughout the day, he propped her upright, then on her belly over a pillow, and gently patted her back and chest for over an hour to stimulate her lungs and loosen up the mucus in her airways. It worked; Jade was able to stay off the ventilator.
“When people give you such a generous gift of their time like that, you sense their sacrifice and truly feel blessed,” Courtney said.
That Thursday was Thanksgiving. While Jade rested in the PICU, her parents went down to the cafeteria to eat dinner.
“That ended up being a life-defining moment for us,” Courtney recalled. “When you’re at home for Thanksgiving, it’s easy to get overwhelmed by the small stuff – the casserole and green beans and rushing off to this or that place. But sitting in that cafeteria, I have never been more thankful in my entire life. You feel humbled and become aware of what matters so clearly. We decided right then that we would come back to the cafeteria every Thanksgiving with our family.”
Remembering with gratitude
mother, Courtney, in spring 2018.
Jade ended up spending eight days in the PICU, followed by six days in a nearby acute care unit, where she continued to receive excellent care. When she got the ‘all clear’ to take Jade home, Courtney stopped in the PICU to let Jade’s care team know and to thank them.
“It was amazing to see Jade transition from this limp baby to this alert little girl, looking around and being so full of life,” Kenley said.
Once home, it took Jade about three months to fully recover from her bout with infant botulism. “Today, she is as normal and healthy as any child could be,” Courtney said. “The botulism is just a piece of her medical history – not the end of her story.”
When the Watts family has since returned to Kentucky Children’s Hospital, it has been by choice rather than in an emergency. For National Nurses Week, Courtney brought Jade with her to drop off care packages for the PICU nurses.
She also took the occasion to write up a letter praising Kenley that she posted on Facebook. When the staff at Kentucky Children’s Hospital caught wind of the letter, they included it in their nomination of Kenley for the Daisy Award for Extraordinary Nurses. She won. “It’s so humbling for someone to be that grateful for your care,” Kenley said.
On Thanksgiving night, the Watts family returned again, as they pledged on that life-altering night one year before. They ate in the cafeteria and they dropped off another round of appreciation gifts for the PICU staff. This time, there was a special note attached from Jade, saying, “Happy Thanksgiving, PICU Friends!”





