Degenerative disc disease
Degenerative disc disease (DDD) is not really a disease but a term used to describe the normal changes of the discs in the spine as a person ages. The breakdown of the discs can result in back pain, neck pain, or other problems.
Age-related changes that cause DDD include a loss of fluid in the discs and tiny tears or cracks in the outer layer (annulus or capsule) of the disc. A sudden (acute) injury leading to a herniated disc may also begin the degeneration process.
Pain from DDD is first treated with ice or heat and with over-the-counter medicines. If you develop health problems such as osteoarthritis, a herniated disc, or spinal stenosis, you may need other treatments. These include physical therapy and exercises. In some cases, surgery may be recommended.
Symptoms
What are the symptoms of degenerative disc disease?
Many people with degenerative disc disease have no pain. But others have severe pain or other symptoms that limit their activities. Some of the most common symptoms are:
- Pain in the back or neck. Where the pain occurs depends on which discs are affected.
- Pain that gets worse when you move, such as when you bend over, reach up, or twist.
- Pain that may occur in the rear end (buttocks), arm, or leg if a nerve is pinched.
- Numbness or tingling in your arm or leg.
The pain may start after a major injury (such as from a car accident), a minor injury (such as a fall from a low height), or a normal motion (such as bending over to pick something up). It may also start gradually for no known reason and get worse over time.
Discs of the Spine
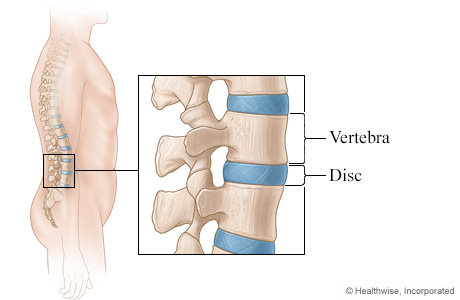
The spine is formed by 33 interlocking bones called vertebrae. Located between each pair of vertebrae is a disc. The disc is composed of a capsule of connective tissue surrounding a soft, jellylike center. These discs absorb shock and provide flexibility within the spine.
Diagnosis
How is degenerative disc disease diagnosed?
A doctor can often diagnose degenerative disc disease while doing a physical exam. If your exam shows no signs of a serious condition, imaging tests (such as an X-ray) aren't likely to help your doctor find the cause of your symptoms.
Sometimes degenerative disc disease is found when an X-ray is taken for another reason, such as an injury or other health problem. But even if the doctor finds degenerative disc disease, that doesn't always mean that you will have symptoms.
Causes
What causes degenerative disc disease?
As we age, our spinal discs break down, or degenerate. This breakdown causes the symptoms of degenerative disc disease in some people.
When the discs break down, they can lose fluid and dry out, and their outer layers can have tiny cracks or tears. This leads to less padding and less space between the bones in the spine. The body reacts to this by making bony growths on the spine called bone spurs. These spurs can press on the spinal nerve roots or spinal cord. This can cause pain and can affect how well the nerves work.
These changes in the discs are more likely to occur if you smoke, do heavy physical work (such as repeated heavy lifting), or are very overweight. A sudden injury may also cause changes to occur.
Treatment
Caring for yourself when you have degenerative disc disease
Here are some things you can do to help manage pain from degenerative disc disease.
- Use ice or heat (whichever feels better) on the affected area.
- Put ice or a cold pack on the area for 10 to 20 minutes at a time. Put a thin cloth between the ice and your skin.
- Put a warm water bottle, a heating pad set on low, or a warm cloth on your back. Put a thin cloth between the heating pad and your skin. Do not go to sleep with a heating pad on your skin.
- Ask your doctor if you can take an over-the-counter pain medicine.
These include acetaminophen (such as Tylenol) and nonsteroidal anti-inflammatory drugs, such as ibuprofen or naproxen. Be safe with medicines. Read and follow all instructions on the label.
- Get some exercise every day.
Exercise is one of the best ways to help your back feel better and stay better. It's best to start each exercise slowly. You may notice a little soreness, and that's okay. But if an exercise makes your pain worse, stop doing it. Here are things you can try:
- Walking. It's the simplest and maybe the best activity for your back. It gets your blood moving and helps your muscles stay strong.
- Exercises that gently stretch and strengthen your stomach, back, and leg muscles. The stronger those muscles are, the better they're able to protect your back.
Copyrighted material adapted with permission from Healthwise, Incorporated. This information does not replace the advice of a doctor.
