Splinting or Bracing
Wearing a splint: Overview
A splint protects a broken bone or other injury. If you have a removable splint, follow your doctor’s instructions and only remove the splint if your doctor says it’s okay.
Most splints can be adjusted. Your doctor will show you how to do this and will tell you when you might need to adjust the splint. A splint is sometimes called a brace. You may also hear it called an immobilizer. An immobilizer, such as a splint or cast, keeps you from moving the injured area.
You may get a splint that’s already factory-made. Or your doctor might make your splint from plaster or fiberglass. Some splints have a built-in air cushion. Air pads are inflated to hold the injured area in place.
Counterforce brace
A counterforce brace is a strap worn around the forearm just below the elbow and used primarily for tendon problems. Some health professionals believe that the brace distributes pressure from muscle use throughout the area, rather than just on the tendon.
Night splint
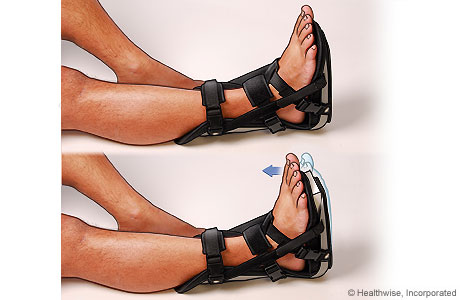
Night splints (braces) may be used to treat conditions such as Achilles tendinopathy and plantar fasciitis. The splint holds the foot with the toes pointed up. This position applies a constant, gentle stretch to the plantar fascia. It also stretches the Achilles tendon at the back of the heel, preventing it from contracting. You can wear night splints every night for up to several months. Then you can gradually reduce how often you use them as your symptoms go away.
The brace usually is adjustable, so you and your doctor can adjust it to the proper angle. There are many types of braces. This picture shows one style.
While you use night splints, you can continue other treatment with nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy, or orthotic devices.
Wrist splint
A wrist splint is a brace that looks like a fingerless glove. It stabilizes the wrist in a straight and sometimes slightly bent-back position. A wrist splint can be worn to support the wrist while holding it firm and still (immobilizing it).
A good wrist splint should:
- Be comfortable, washable, durable, and easy to remove.
- Keep the wrist in a neutral position. The wrist is generally in a neutral position when the person is holding a glass of water, with the thumb in line with the forearm.
- Restrict wrist movements while allowing fine hand movements, such as writing or typing.
Splints are available without a prescription from a drugstore or with a prescription from an orthopedic or medical supply house. Physical and occupational therapists can custom-fit splints made from lightweight materials. Health professionals usually do not recommend long-term use of splints (more than 72 hours) because the muscles in the hand or wrist can become weak.
Pavlik Bracing
Pavlik harness
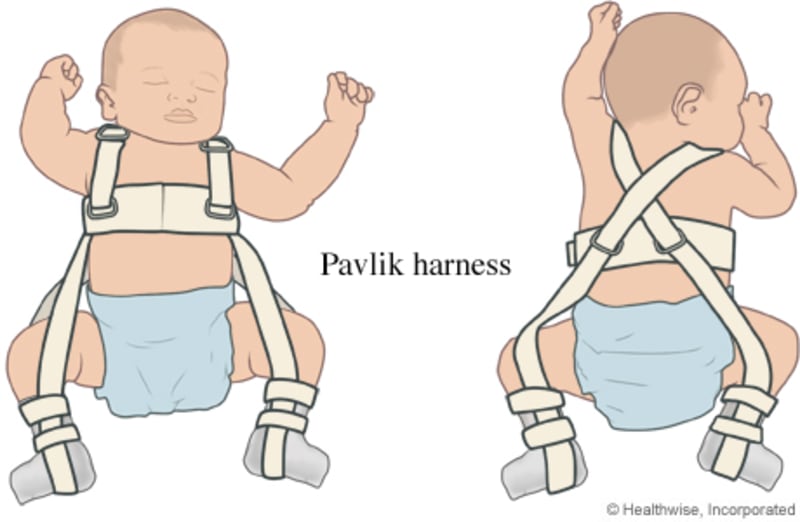
A Pavlik harness is a brace often used to treat developmental dysplasia of the hip (DDH) in babies younger than 6 months.
The harness has fabric straps and fasteners that fit around a baby's chest, shoulders, and legs. The harness holds the baby's legs in a spread position, with the hips bent so that the thighs are out to the sides. This keeps the head of the thighbone (femur) in the correct position in the hip socket for normal development.
Self-Care
How can you care for yourself when you wear a splint?
General care
- Follow your doctor's instructions on how much weight you can put on your injured limb.
- If the fingers or toes on the limb with the splint were not injured, wiggle them every now and then. This helps move the blood and fluids in the injured limb.
- Prop up the injured limb on a pillow when you ice it or anytime you sit or lie down during the next 3 days. Try to keep it above the level of your heart. This will help reduce swelling.
- Put ice or cold packs on the limb for 10 to 20 minutes at a time. Try to do this every 1 to 2 hours for the next 3 days (when you are awake) or until the swelling goes down. Be careful not to get the splint wet. Put a thin cloth between the ice and your skin. If your splint is removable, ask your doctor if you can take it off when you use ice.
- If you have an adjustable splint that feels too tight, loosen it slightly.
- Keep up your muscle strength and tone as much as you can while protecting your injured limb. Your doctor may want you to tense and relax the muscles protected by the splint. Check with your doctor or your physical or occupational therapist for instructions.
Splint and skin care
- If your splint is not to be removed, try blowing cool air from a hair dryer or fan into the splint to help relieve itching. Never stick items under your splint to scratch the skin.
- Do not use oils or lotions near your splint. If the skin becomes red or sore around the edge of the splint, you may pad the edges with a soft material, such as moleskin, or use tape to cover the edges.
- If you're allowed to take your splint off, be sure your skin is dry before you put it back on. Be careful not to put the splint on too tightly.
- Check the skin under the splint every day. If you can't remove the splint, check the skin around the edges. Tell your doctor if you see redness or sores.
Water and your splint
- Keep your splint dry. Moisture can collect under the splint and cause skin irritation and itching. If you have a wound or have had surgery, moisture under the splint can increase the risk of infection.
- Tape a sheet of plastic to cover your splint when you take a shower or bath, unless your doctor said you can take it off while bathing.
- If you can take the splint off when you bathe, pat the area dry after bathing and put the splint back on.
- If your splint gets a little wet, you can dry it with a hair dryer. Use a "cool" setting.
When to Call
Wearing a splint: When to call
Call your doctor now or seek immediate medical care if:
- You have increased or severe pain.
- You feel a warm or painful spot under the splint.
- You have problems with your splint. For example:
- The skin under the splint is burning or stinging.
- The splint feels too tight.
- There is a lot of swelling near the splint. (Some swelling is normal.)
- You have a new fever.
- There is drainage or a bad smell coming from the splint.
- Your limb turns cold or changes color.
- You have trouble moving your fingers or toes.
- You have symptoms of a blood clot in your arm or leg (called a deep vein thrombosis). These may include:
- Pain in the arm, calf, back of the knee, thigh, or groin.
- Redness and swelling in the arm, leg, or groin.
Watch closely for changes in your health, and be sure to contact your doctor if:
- The splint is breaking apart or losing its shape.
- You are not getting better as expected.
Copyrighted material adapted with permission from Healthwise, Incorporated. This information does not replace the advice of a doctor.
