A Spark for Life

Breanna Jessie’s feisty spirit has long been her best medicine in dealing with cystic fibrosis. But when the disease devastated her lungs, she got a second chance at life thanks to the experts at UK HealthCare.
A firecracker. A spitfire. That is how Breanna Jessie’s care team members at UK HealthCare consistently describe this one-of-a-kind 20-year-old young woman who has battled cystic fibrosis (CF) her whole life. Diagnosed at the age of 3, Breanna has always drawn on her trademark high energy and gutsy determination in facing CF’s increasing impairment of her respiratory and digestive systems.
Never were they needed more than when the calendar rolled over into 2018 and CF pushed Breanna’s lungs to their limit. Over the next intense and precarious four months, Breanna’s care team rallied their patient’s feisty spirit and their own significant expertise – particularly in the leading-edge ECMO heart-lung bypass treatment – to keep Breanna alive and healthy enough to qualify for a double-lung transplant.
A childhood with CF

Cystic fibrosis is a rare genetic disease that affects around 30,000 patients in the U.S., according to the Cystic Fibrosis Foundation. It causes a patient’s mucus to be thick and sticky, clogging airways and raising the risk of respiratory infections. The mucus also affects the release of digestive enzymes from the pancreas, blocking the absorption of important nutrients by the body.
Soon after Breanna turned 3, her parents, Dave and Debra, noticed she was having difficulty breathing and digesting food. They made the wintry 85-mile drive west from their home in the small rural town of Olive Hill to Lexington for a consult at Kentucky Children’s Hospital. Jamshed Kanga, MD, chief of pediatric pulmonology, administered a sweat test. It detected high levels of chloride – a hallmark of cystic fibrosis. Shortly after, Debra gave birth to twin boys – Hunter and David – who were soon diagnosed with CF as well. “It was very heartbreaking for the family,” said Dr. Kanga. “Within a three-month period, they had three children with a CF diagnosis.”

Breanna’s earliest memories of living with CF are of having to stay inside most of the time to avoid pollen and other environmental triggers for her coughing spells. “I learned a lot of board games at a young age,” she said. Twice a day, every day, Breanna had to sit still for an hour for vest therapy, otherwise known as high-frequency chest wall oscillation. She would put on an inflatable vest under her clothes and attach it, via two hoses, to a machine. The machine vibrated the vest at a high frequency to thin out and loosen mucus in her chest, which she would then cough up. “I’d just sit there and shake,” she said.
She also took daily doses of digestive enzymes to help her body better absorb the nutrients in her food. “Keeping on weight was the most important thing,” she said. “If my weight was up, then my breathing was up, too. I could eat anything I wanted just to gain weight.”
Her health stayed relatively stable until the end of eighth grade, when she was hospitalized with the flu. She lost half of her right lung, and her blood-oxygen saturation dropped from 90 percent to 75 percent or lower. During high school, she developed pseudomonas, a bacterial infection that can be debilitating to the lungs. Breanna bristled at having to be hospitalized more often.
“She has never been a patient who would lie down and just do everything the doctor told her to do,” said Kanga. “She would ask, ‘Why?’ or say, ‘This doesn’t work with my routine.’ She has always had some rebelliousness in her. I think that is what keeps these CF patients going. They are the most stubborn kids in the world. They have this will to live that keeps them going.”
Despite her hospitalizations, Breanna was determined to make the most of high school. She participated in Future Farmers of America (FFA), took engineering classes, attended the homecoming dance and even made the dance team.
“She came to the clinic one day and I told her, “You’re sick. Your lung function is way down,’” said Kanga. “She said, ‘I’m just fine. Let me show you what I did yesterday.’ And she showed me one of her routines from a dance competition. She was going 100 miles an hour. You wouldn’t know there was anything wrong with her. But she had such bad lung function that we took her straight from the clinic to the hospital.”
At the end of her junior year, Breanna’s condition took a serious turn. “We had to keep sizing down my prom dress because I was losing so much weight,” she said. Two days after prom, she collapsed at a local festival. By the time she arrived at Kentucky Children’s Hospital, she was coughing up a large amount of blood. Abnormal blood vessels become enlarged in the damaged area of lung in cystic fibrosis and can develop dangerous bleeding. These vessels had to be blocked off by the interventional radiology team to prevent her from bleeding to death. She slowly recovered after the procedure, but it seemed to be the start of a more rapid decline in her health.
“My lung function just kept going down, down, down after that,” Breanna said. “All I wanted was to be able to graduate from high school.” She did, on time. But soon afterward, she entered a tailspin as her condition progressed to end-stage lung disease. She started skipping breathing treatments as she tried to keep up with college classes and help take care of her brothers. At the boys’ 16th birthday party, on December 29, 2017, Breanna was too exhausted to walk; her blood-oxygen saturation level was barely 50 percent. She was rushed to UK Albert B. Chandler Hospital, where she would remain for the next four months.
Rallying the resources and can-do spirit
The top priority of the care team in the pulmonary intensive care unit (ICU) was to stabilize Breanna’s breathing. “She was in a lot of respiratory distress,” said Michael Anstead, MD, FCCP, medical director of the Center for Lung Transplant and director of the Adult Cystic Fibrosis Center. “Over several days, even though she received antibiotics and steroids, her condition got worse, so we placed her on a ventilator.” She also had a tracheostomy, a procedure that puts a tube through a hole in the patient’s neck so that the ventilator can pump air directly into the windpipe.

Breanna’s lungs were too stiff to respond well enough on the ventilator, so she soon was also put on ECMO (extracorporeal membrane oxygenation). This heart-lung bypass treatment uses a catheter to move blood out of the body and into an external pump. The blood circulates through an artificial lung to be scrubbed of carbon dioxide and “recharged” with oxygen and then is sent back into the patient’s bloodstream.
ECMO requires around-the-clock support from a highly coordinated team, ranging from specialized nurses to physicians to respiratory, physical and occupational therapists. “It can be a lifesaving treatment,” Dr. Anstead said.
It also can have its complications. “ECMO can chew up a patient’s blood cells, and so they often need blood transfusions,” Anstead explained. “Because of those transfusions, Breanna’s body started making antibodies that would have caused complications for a transplant.” In early February, she was taken off ECMO to give her body time to purge the antibodies.
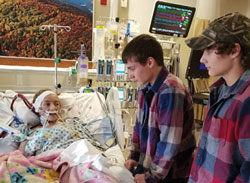
Breanna’s memories are fuzzy of her first six weeks in the ICU. She remembers “coming to,” as she puts it, on February 14 – Valentine’s Day. She received a flood of texts from friends, family, even high school coaches sharing messages of love and support. “It was overwhelming to know how many people cared,” she said.

Breanna’s brothers, Hunter and David, were relieved to see her fully awake. “Hunter asked me, ‘Are you going to be okay?’” she remembered. “I told him, ‘It’s all going to be okay, I promise.’ I made a pinkie promise with him that it would be okay.”
Anstead had a frank discussion with Breanna about her prognosis. “He told me, ‘You won’t walk out of this hospital without a new set of lungs,’” she recalled. He also told her that if she wanted to be on the lung transplant list, she needed to walk. Research shows that transplant patients who can walk 300 feet prior to their surgery have much better outcomes.
Breanna was skin and bones with no muscle tone. Enter physical therapist Kathryn Gaines, PT, DPT. It was her job to get Breanna up and moving, one step at time, along the ICU hallways and toward her goal of a lung transplant.
“Every time I went to get her, she’d say, ‘I am not going to do it,’” Gaines said. “But she would rally herself and make herself do it.” Breanna would crank up the Carrie Underwood song “The Champion” on her phone and force herself to walk a little farther with each session. A chart in Breanna’s room documented how many feet she covered each time. “She could see she was making progress,” Gaines said. “It was possible; she could do it.” She did. And she was put on the transplant list.
Another member of Breanna’s team who took care to the next level was respiratory therapist Anne Fitzpatrick, RRT. “She was always there by my side,” Breanna said.

Fitzpatrick monitored Breanna’s ventilator settings. She provided nebulization treatments to break apart the mucus. And when mucus plugged Breanna’s airways, Fitzpatrick “blocked” her, squeezing a bag valve to manually force air into her lungs.
“She would work with my breath instead of against it,” Breanna explained. “If something wasn’t quite right, she’d adjust and it would be perfect.”
As a frequent presence in Breanna’s room, Fitzpatrick soon became a comforting companion as well, especially during those times when Breanna’s family members could not be with her. “I’d keep her company, even on my days off,” Fitzpatrick said. “I knew it gave her a calmness she needed.”
“I can hold on a little bit longer.”
It was a calm amidst the storm. With each passing week, the care team did their best to keep Breanna strong in body and spirit. One day Fitzpatrick wheeled Breanna outside for a respite from her hospital room. “I wanted her to feel the sunshine one more time in case she didn’t make it,” Fitzpatrick said. But the sun did not cooperate, and the cool and windy weather quickly drove them back inside.
Breanna’s respite from ECMO was over as well. “Her lungs were at the point of failing,” Fitzpatrick said. “Her CO2 levels got so high that the pressure was causing migraines and making her eyes bulge. She had to go back on ECMO a second time, which is unheard of.”
The following week, on April 11, the news came that Breanna had been waiting for: She had been matched with a donor, a 25-year-old male. “I couldn’t believe it,” she said. But after preliminary surgery prep, she waited…and waited. Then she was told that the surgeons had rejected the lungs. The transplant was canceled.
“It happens fairly often,” Anstead explained. “In this case, some of the blood vessels were damaged and there would have been trouble sewing in the donor lungs. We had to turn down the match.”
Breanna’s family members cried around her bedside. “I heard this little voice in my head that said, ‘Tell them you’re going to be okay – that you’re not going anywhere,’” Breanna said. “That’s what I did. I told my dad, ‘It’s going to be okay. I can hold on a little bit longer.’”
That is all it took – a little bit longer. Two days later, on April 13, Breanna was matched with another donor: a young woman her age and her build with healthy lungs. “This was the perfect set of lungs for someone in Breanna’s situation,” Anstead said.
This time, Breanna gave herself permission to cry, too. “I was so happy,” she said. “My mom and my aunt and I watched through the window as the helicopter flew over.” She was quickly wheeled to the operating suite, where the transplant team began the eight-hour surgery.
“I have things to do now.”
Breanna was expected to sleep for two days after surgery; instead she woke up within hours. “The doctor came in and said, ‘What in the world? How are you awake already?’” she recalled. “I told them, ‘I’m not tired. I don’t need to sleep.’ They told me that in order to get out of the recovery room I had to walk. So I did; I walked half of the hallway with my dad.”
Her appetite quickly came roaring back. “The day after she got her lungs, she ate a whole plate of chicken, mashed potatoes, and mac and cheese,” Fitzpatrick said with a laugh. “I don’t know if she chewed it or swallowed it whole. Her whole body was hungry again.”

After her transplant, Breanna’s care team added new members: Maher Baz, MD, medical director of lung transplant, would now be her primary physician. And Rachael Serafini, BSN, became her lung transplant coordinator, her first point of contact for all questions and care going forward. They quickly became acquainted with Breanna’s feisty side.
“She was on the go after her transplant, ready for the next phase,” said Dr. Baz. “She’d say, ‘I need to get back on my feet, learn my meds, learn how to take care of myself. I have things to do now.’”
About a week after the surgery, she was taken off the ventilator for the first time in four months. She took her first breath on her own with her new lungs. “It was amazing,” she said. “I love country music, but I could never finish a song without getting out of breath. So I sang a whole song, all the way to the end. That was life changing.” The song: Carrie Underwood’s “The Champion.”
She was strong enough to transition to a nearby hotel on May 2 for her last month of medical supervision. Friends came to visit and lift her spirits, especially through some challenges. She contracted MRSA, a drug-resistant infection that is always a concern but especially so for a recent transplant patient. She also suffered a seizure a week before she was to be discharged. But true to form, she persevered, and she was sent home just two days behind schedule, on June 1 – 154 days after she arrived. The next day, she cheered on a close friend at his high school graduation, just as she had promised she would.

Breanna will never have a completely clean bill of health. Her cystic fibrosis continues to affect her digestive system and pancreas. She has developed diabetes, common for CF patients, and now needs to watch what she eats – a tough lifestyle change for someone who has always eaten whatever she wanted in order to gain weight.
She has been hospitalized a few times for rejection and infection. Each time she pushed to be released as soon as possible. “You just have to lay out the bigger picture for her,” Serafini said. “The last thing she wants is to go back in the hospital. But if we tell her about the positive results that await if she gives us five days to straighten her out, she can do that.”
This spring, Breanna reached the one-year anniversary of her transplant, a major milestone. “She is doing great,” said Fitzpatrick, who remains a close friend of Breanna’s. “She’s a firecracker who won’t let anything stop her.”
From now on, Breanna’s checkups will be fewer and farther between. That is just fine with her because she has people to see and things to do to make up for all those lost years. “I can play basketball,” she said. “I can run with my friend’s little girls and keep up with them. I can be outside and be around animals and not have to worry anymore. I can get out and live.”






